Blood Donor Shortage Worsens as Artificial Substitutes Remain Limited to Emergency Use
A critical shortage of blood donors, particularly those with universal O-negative type, persists due to declining participation and demographic shifts, while artificial blood substitutes like ErythroMer remain years away from replacing human donations for most medical needs.
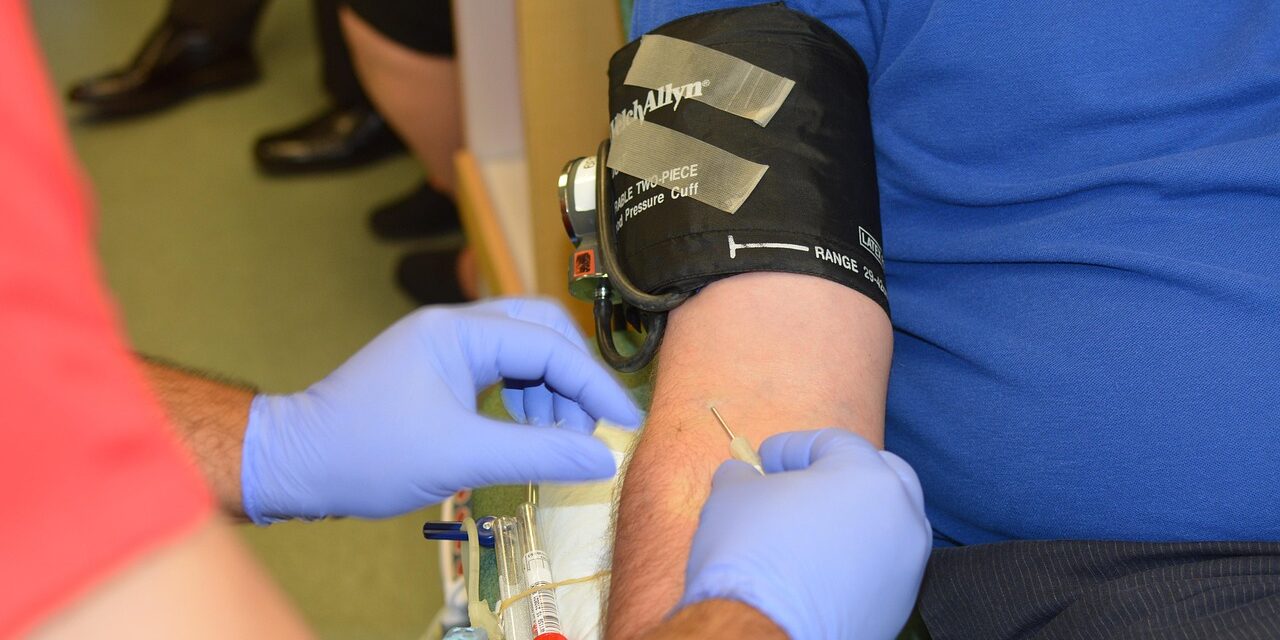
The American Red Cross faces a severe and worsening shortage of blood donors, particularly those with O-negative blood type, which serves as universal donor blood for emergencies when a patient's type is unknown. Only about 3% of the U.S. population donates blood annually to supply 13.6 million units of whole blood and red blood cells needed for medical treatments. O-negative Red Blood Cells have been in chronic short supply since 2021, with supply challenges intensified by a declining donor base and changing donor demographics.
According to the Red Cross, the COVID pandemic curtailed blood drives and many have not resumed, while younger generations are not donating at the same rates as their elders. This trajectory is considered unsustainable for maintaining adequate blood supplies. The shortage is particularly acute for O-negative donors, who represent just 7% of the population but provide blood that can be given to anyone, from premature babies in the NICU to trauma victims.
Researchers have been working for 80 years to develop artificial blood substitutes, but progress has been slow. A research center at the University of Maryland medical school in Baltimore, along with company KaloCyte that emerged from that research, has developed ErythroMer, a powdered substitute that can be mixed with water to create a liquid with some blood-like qualities. However, as Dr. Allan Doctor, head of the Center for Blood Oxygen Transport & Hemostasis at the University of Maryland School of Medicine explains, this product serves only as "a bridging therapy" for bleeding emergencies outside hospitals.
Dr. Doctor, who was recruited to Maryland six years ago to run the center and bring KaloCyte to market, told WJZ TV that ErythroMer is designed to save the approximately 30,000 people who bleed out annually before reaching hospitals, noting that "you can't give transfusions in the field right now." Even if approved for human use, artificial substitutes will not solve the overall blood shortage problem, as patients will still need human blood with all its complex properties that researchers have been unable to duplicate artificially.
The Red Cross, which collects 40% of the country's blood supply, is attempting to enhance the donor experience to encourage more donations. The organization is conducting trials of a new device that eliminates the finger-stick hemoglobin test by passing light through the thumb instead. While this reduces pain and supply costs, the technology has limitations - if the hand isn't warm enough, readings can be inaccurate, potentially causing eligible donors to be rejected. The agency provides small warmer packs as a workaround, but technical challenges remain.
Qualifying to donate blood requires meeting basic criteria: weighing at least 110 pounds, being 17 years old, and having no tattoos, piercings, intravenous drug use, or paid sexual activity within the past year, among other medical conditions. The donation process, including screening and recovery, typically takes about two hours for power red donations (which provide double the red blood cells) every 112 days, or 56 days between whole blood donations.